Structural Heart Disease
Frontier Explorer
STRUCTURAL HEART DISEASE
Recently, the 6th session of the “Yujun ValveCare · Transapical Excellence” TEER (Transcatheter Edge-to-Edge Repair) Hands-on Training Camp, organized by Hangyu Medical, was successfully held in Changsha, Hunan Province.
As the first TEER practical training camp in Central China, the event brought together over 60 experts and physicians from 16 medical centers across Hunan Province, representing cardiovascular surgery, interventional cardiology, echocardiography, and perioperative nursing.
Through systematic theoretical courses, real-case discussion, and simulation-based hands-on practice, the program aimed to promote standardized TEER practice and strengthen team-based collaboration across the region.


Opening Remarks: A Milestone for TEER Development in Hunan
The training camp opened with an inspiring address by Professor Zhao Yuan from the Second Xiangya Hospital of Central South University. Prof. Zhao warmly welcomed attendees and emphasized the clinical value and bright future of TEER technology. He noted that hosting this hands-on training camp represents a key step toward standardized TEER adoption and clinical integration in Hunan.
He highlighted that high-level academic platforms such as this one help:
advance knowledge exchange between provincial and local centers,
support the downward extension of cutting-edge technologies, and
elevate overall structural heart disease management, ultimately benefiting a greater number of patients.

The curriculum was designed around the core workflow of TEER, led by experts from the Second Xiangya Hospital.

 Prof. Cao presented the surgical philosophy of mitral valve repair, emphasizing that repair is superior to replacement. Valve replacement disrupts native subvalvular structures and adversely affects long-term ventricular function, while repair preserves valve anatomy and restores physiological mechanics, leading to near-normal postoperative function.
Prof. Cao presented the surgical philosophy of mitral valve repair, emphasizing that repair is superior to replacement. Valve replacement disrupts native subvalvular structures and adversely affects long-term ventricular function, while repair preserves valve anatomy and restores physiological mechanics, leading to near-normal postoperative function.
He highlighted:
Repair should always be considered first: “If it can be repaired, repair it — repair is better than replace.”
TEER shares the same foundational principle as surgical repair: restoring leaflet coaptation, eliminating MR, and maintaining adequate valve area.
Prof. Cao analyzed the fine anatomy of the mitral valve and described tailored repair strategies for different lesion types (anterior, posterior, commissural), including triangular resection, quadrangular resection, neochordae implantation, annuloplasty band selection, edge-to-edge suturing, and saline testing.
He summarized the four core criteria of successful repair:
No MR
No stenosis
Adequate coaptation height
Proper coaptation position
 Prof. Wu delivered a comprehensive lecture on the central role of echocardiography in TA-TEER.
Prof. Wu delivered a comprehensive lecture on the central role of echocardiography in TA-TEER.
She emphasized that ultrasound is not only the “eyes” of the operator but also the navigation system enabling precise and reproducible repair.
Key points included:
Aortic valve = 12 o’clock
Left atrial appendage = 9 o’clock
Posterior commissure = 3 o’clock
This ensures alignment between the echocardiographer’s language and the surgeon’s spatial interpretation.
She detailed MR mechanism identification and quantification using:
PISA, CW vena contracta
AP annular diameter
Leaflet length
Coaptation index (CI)
Leaflet-to-annulus index (LAI)
and differentiated PMR (degenerative) vs SMR (atrial/ventricular functional) with clear imaging indicators.
Ultrasound provides real-time navigation for:
Skin entry and intercostal approach
Apical puncture trajectory
Transapical system advancement
Clip positioning and leaflet capture
She emphasized the “4M Rule”:
Morphology (valve structure)
MR (residual regurgitation)
Mean Gradient
Mechanism (grasping quality)
Prof. Wu also reviewed chordae classification, key TEE views, Mitral valve clock-face orientation (surgeon’s view), and new leaflet types (interlaced, symmetric, Y-shaped, oblique-hook types).
Through two representative cases (PMR and SMR), she demonstrated the complete process of preoperative evaluation → intraoperative imaging → immediate post-clip assessment.
She concluded that with the rapid expansion of TA-TEER in China, ultrasound is evolving from an “assistive tool” to a co-creator of the procedure, and only standardized, unified communication between imaging and surgical teams enables true procedural precision.
3. “Perioperative Nursing Collaboration in Complex Cardiac Surgery” — Prof. Lin Gang
Professor Lin Gang, from the perspective of nursing management, systematically introduced the team composition and key perioperative nursing points in complex cardiac surgeries. He provided a detailed explanation of preoperative patient preparation, the setup of interventional and surgical instruments as well as sophisticated equipment, and the optimization of operating room layout. He also elaborated on the precise collaboration between scrub nurses and circulating nurses during procedures, emphasizing the critical role of nursing within the multidisciplinary team (MDT) in ensuring patient safety and improving surgical efficiency.

4. Product Presentation and Interactive Discussion — Hanyu Medical Technical Department
The technical team from Hanyu Medical delivered an in-depth introduction to the ValveClamp® Mitral Valve Clip System and its procedural workflow, covering device features, preoperative preparation, and key surgical steps such as apical puncture and positioning, transvalvular passage, clamping, and release. They also explained the intraoperative assessment criteria based on the “4M Principle,” providing participants with a clear understanding of the device and a solid theoretical foundation for its operation.

 Professor Zhao Yuan vividly demonstrated the practical application of TA-TEER (Transapical Transcatheter Edge-to-Edge Repair) through three representative complex clinical cases. He focused on sharing his experience in developing individualized surgical strategies based on preoperative TEE assessments—such as choosing between single or dual clip implantation and planning the optimal placement.
Professor Zhao Yuan vividly demonstrated the practical application of TA-TEER (Transapical Transcatheter Edge-to-Edge Repair) through three representative complex clinical cases. He focused on sharing his experience in developing individualized surgical strategies based on preoperative TEE assessments—such as choosing between single or dual clip implantation and planning the optimal placement.
Professor Zhao summarized key procedural points and risk-avoidance techniques, including maintaining coaxial alignment during apical puncture, ensuring stable leaflet capture, and preventing chordae entanglement. His insights clearly illustrated the core value of the “4M Principle” in guiding procedural success.
Through real clinical demonstrations, Prof. Zhao showcased the feasibility and efficacy of TEER across different etiologies (DMR/VFMR) and complex lesions, emphasizing that collaborative decision-making among imaging, surgery, and the heart team is the cornerstone of success.
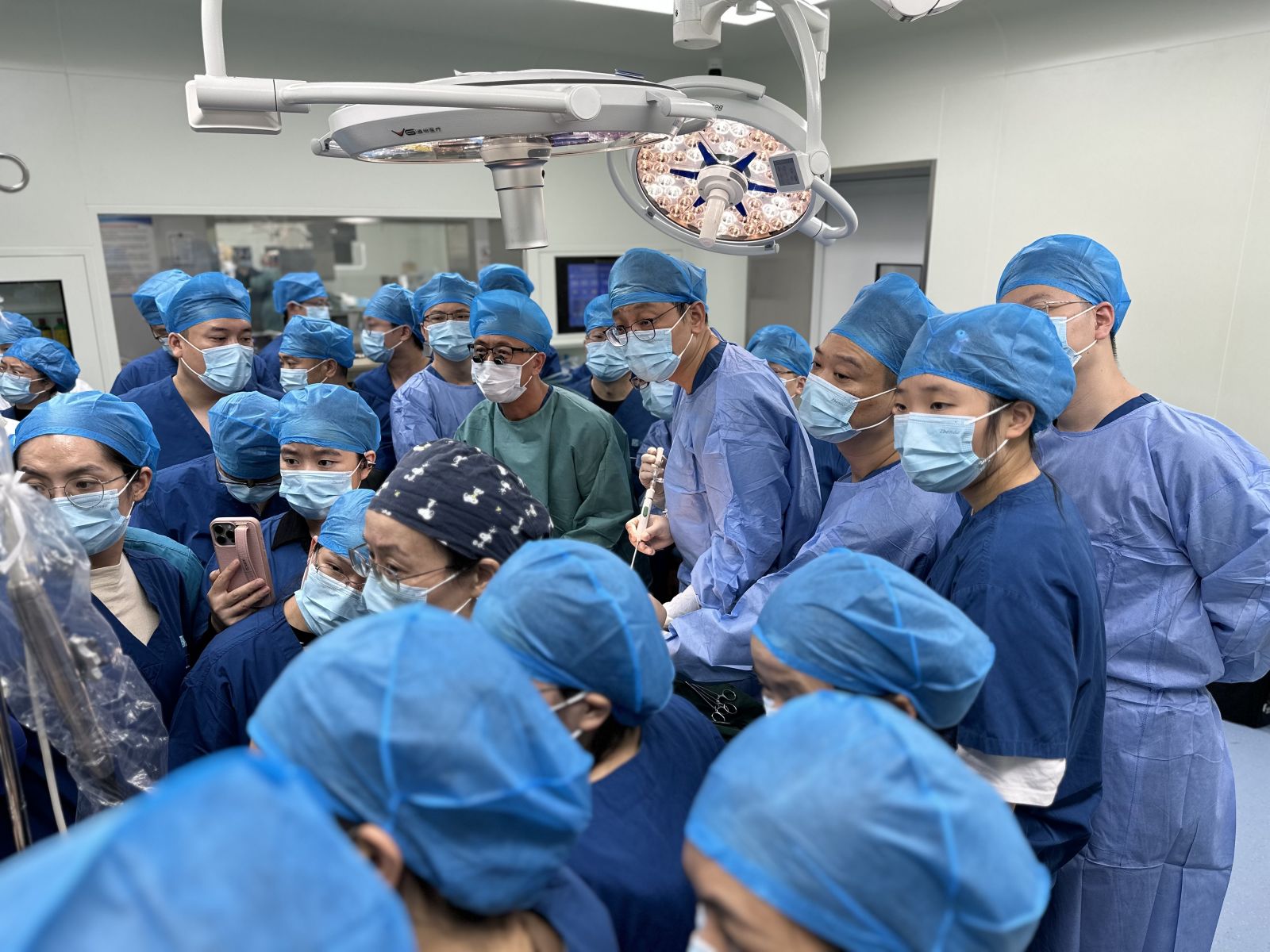
Building on the solid theoretical foundation, the training camp incorporated simulated procedural sessions. Under expert guidance, participants practiced each procedural step—from apical puncture and device delivery to leaflet grasping and clip deployment.
This hands-on, mentorship-driven teaching model greatly deepened participants’ understanding of the procedural essentials, enhancing team coordination and imaging interpretation skills in real-world scenarios.
At the close of the event, Mr. Wang Hui, CEO of Hanyu Medical, presented certificates of completion to all participants, followed by a group photo to commemorate the achievement.
The successful completion of this training camp not only provided cardiovascular interventional physicians across Central China with a high-level learning and exchange platform, but also marked a new stage in the standardized training and regional promotion of TEER technology.



Looking Ahead
Moving forward, Hanyu Medical will continue to collaborate with leading medical centers nationwide to deepen education and training initiatives, helping to advance China’s overall capabilities in structural heart disease interventions and to bring minimally invasive, precision therapies to more patients in need.